Cardiac-SPECT
Principal Investigator: Scott D. Metzler
Background
About 80 million American adults (1 in 3) have one or more types of cardiovascular disease with an annual mortality currently exceeding 500,000 per year. The direct and indirect costs from cardiovascular disease and stroke are estimated at about $450 billion/year, with coronary heart disease accounting for about $150 billion.
Myocardial Perfusion Imaging (MPI) measures how well blood is nurishing the heart muscle (the myocardium). Various techniques can be used for this measurement including Magnetic Resonance Imaging (MRI) and the nuclear-emission modalities of Positron Emission Tomography (PET), and Single Photon Emission Computed Tomography (SPECT).
In these nuclear techniques, a small amount of radioactive tracer is injected and accumulates preferentially in the heart. The tracer decays and emits gamma rays that are detected by the surrounding scanner. This, in some ways, is like an x-ray from the inside out showing how the heart is functioning.
The most commonly used technique for MPI is traditional SPECT because of its cost effectiveness and availability. There are currently about 8 million cardiac SPECT scans per year compared to 200,000 cardiac PET scans. MRI is much less frequent.
Traditional SPECT utilizes two large detectors that are separated by 90 degrees. The detectors rotate about the patient. These data are then reconstructed into 3D images showing the tracer distribution in the body.
C-SPECT Design
C-SPECT is a very high-performance cardiac imaging being developed at the University of Pennsylvania. It utilizes a stationary imaging configuration where neither the patient nor the scanner moves. The scanner uses much smaller detectors than a traditional system. These detectors form an arc around the patient that allows collimation to focus on the heart.
C-SPECT uses an adaptive collimation system that allows the underlying system characteristics (slits and slat stacks) to be altered based on the initial images from the patient. This patient-specific approach helps to optimize the overall performance for each scan.
| Slit Conveyor | Slat Stack Collimator |
|---|---|
C-SPECT Status
The initial prototype system is nearing completion. The detector and collimator systems are in place. Characterization studies, including calibration and reconstruction optimization, are underway. Phantom studies will continue through the fall of 2019 with large-animal and patient studies beginning in 2020.

|

|
C-SPECT Phantom Study
Using the Data Spectrum dynamic (beating-heart) phantom placed on a stage to mimic respiratory motion, we have acquired and reconstructed myocardial perfusion data. C-SPECT acquires a set of projections, which are 2D images resulting from the detection on flat, rectangular detectors of gamma rays emitted from the phantom that pass through the collimator. These data are reconstructed to recreate the original 3D distribution
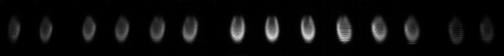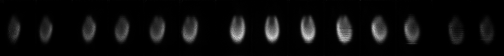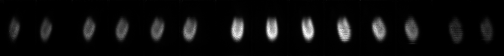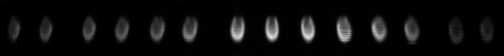
|

|
Selected Presentations
- D. Stentz, L.C. Johnson, P. Sankar, and S.D. Metzler. Demonstration of Duel Gating on C-SPECT for Respiratory Correction in Gated Myocardial Perfusion Imaging. 2019 IEEE Nuclear Science Symposium and Medical Imaging Conference, Manchester, UK.
- P. Sankar, D. Stentz, L. Johnson, W. Chang, J.S. Karp, and S. Metzler. Performance evaluation of resolution/sensitivity variable slats-stack collimator of C-SPECT cardiac scanner. J Nucl Med, vol. 60, suppl. 1, #191.
- S.D. Metzler, P. Sankar, D.J. Stentz, J.S. Karp, L.C. Johnson, and W. Chang. First imaging data with C-SPECT: A dedicated human cardiac SPECT imager. 2018 IEEE Nuclear Science Symposium and Medical Imaging Conference, Sydney, Australia. M-11-02.
- S.D. Metzler, D.J. Stentz, L.C. Johnson, P. Sankar, and M.A. Guerraty. Phantom Evaluation of C-SPECT Performance for Myocardial Perfusion Imaging. 2020 IEEE Nuclear Science Symposium and Medical Imaging Conference, Boston, Massachusetts (Virtual). M-04-01.


