THE NATION'S FIRST MEDICAL SCHOOL TURNS 250
Chronicles the institution’s fascinating history: from its beginning as a few lectures given in borrowed space to the extensive curriculum, research, and multidisciplinary clinical practice within today's University of Pennsylvania Health System. Its colorful prose and images – including many archival documents, paintings and photographs never previously compiled – track the canon of therapies offered to patients, from the 18th century's handful of primitive and sometimes harmful procedures, such as bloodletting, to today's robotic surgery and gene therapy.
Pennsylvania Hospital is founded
1751

Pennsylvania Hospital, Eighth and Pine streets. William Birch print, c. 1800. Founded in 1751 as the first hospital in the Colonies, it also became the first place to provide clinical instruction to the first medical students in what would become the United States. As of 1767, requirements for a Penn medical degree included one year attending the practice of the hospital. Students purchased tickets for hospital privileges, which included use of the library. In 1997, Penn’s long-standing relationship with Pennsylvania Hospital was formalized with the latter’s merger into the University of Pennsylvania Health System. Courtesy Pennsylvania Hospital Historic Collections, Philadelphia
William Shippen Jr.'s Anatomical Drawings
1762
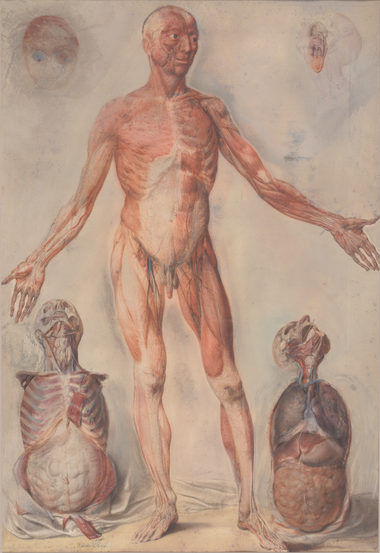
For his anatomy lectures, William Shippen Jr. used anatomical drawings and casts made by the famous Dutch painter, Jan Van Rymsdyk. Before Penn established a medical school, Shippen conducted lectures in anatomy, surgery, bandaging, and midwifery in the Anatomical Theatre, located on his father’s property, today’s 12-14 North Fourth Street. This facility continued to serve as the anatomy laboratory and lecture hall for the new medical school. In the mid-1780s, Shippen built a house on another of his father’s properties at the southwest corner of Fourth and Locust streets. His Anatomical Theatre operated here until the University erected a new building for anatomy and chemistry on Fifth Street in 1791. Courtesy Pennsylvania Hospital Historic Collections, Philadelphia. For his anatomy lectures, William Shippen Jr. used anatomical drawings and casts made by the famous Dutch painter, Jan Van Rymsdyk. Before Penn established a medical school, Shippen conducted lectures in anatomy, surgery, bandaging, and midwifery in the Anatomical Theatre, located on his father’s property, today’s 12-14 North Fourth Street. This facility continued to serve as the anatomy laboratory and lecture hall for the new medical school. In the mid-1780s, Shippen built a house on another of his father’s properties at the southwest corner of Fourth and Locust streets. His Anatomical Theatre operated here until the University erected a new building for anatomy and chemistry on Fifth Street in 1791. Courtesy Pennsylvania Hospital Historic Collections, Philadelphia.
Lecture Ticket
1765

Lecture ticket, 1765. John Morgan, the newly appointed professor of medicine, taught this first course of lectures on materia medica and physic at his house. He handwrote the ticket on the back of an ordinary playing card, a common alternative before printed cards became the norm.
John Morgan, College of Philadelphia
1765

In 1757, John Morgan graduated in the first class of undergraduates from the College of Philadelphia. While an undergraduate, he studied medicine under John Redman and worked at Pennsylvania Hospital as resident apothecary. At the time, this was enough medical training for him to serve as a surgeon during the French and Indian War. He subsequently earned a medical degree at Edinburgh in 1763 and began to formulate his ideas for starting a medical school in Philadelphia. Upon his return in 1765, Morgan presented his proposal to the Trustees of the College of Philadelphia, one of whom was his mentor. The College embraced his concept for a university-based medical school and made him the first professor of medicine in America. Morgan took leave from teaching during the American Revolution to serve as director-general of the Army’s hospital, located in Boston. From 1775 to 1777 he struggled to establish a medical service that was hampered by supply shortages, logistics, an outbreak of smallpox, and a lack of understanding of health issues by Congress and the military. Morgan bore the brunt of blame for the problems. Shippen replaced him, not without controversy. Morgan never returned to teaching, although he resumed his position on the medical staff at Pennsylvania Hospital.
Jonathan Elmer's diploma
1771

Jonathan Elmer’s diploma for a medical degree, 1771. Elmer had been part of the first class of 10 medical students, who in 1768 received their bachelor of medicine degrees. He and three classmates subsequently completed the requisite three years of professional experience and Latin thesis to earn their M.D. diplomas, the first such degrees Penn’s medical school ever awarded. Elmer’s is the only known original of these documents to survive. His great-grandson, Walter Gray Elmer (M 1897), donated it to the University in 1957.
Anatomical Theatre
1791

Anatomical Theatre, Fifth Street, home of the Medical Department’s anatomy and chemistry departments, 1791-1807. The building was also known as Anatomical Hall, The Laboratory, and from William Birch’s 1799 print, Surgeons’ Hall. It became Penn’s and the nation’s first building used exclusively for medical teaching. Two teachers, more than 100 students, and likely several cadavers were crowded into a room no larger than 27 x 35 feet.
Observations Upon the Origin of the Malignant Bilious
1799

Observations Upon the Origin of the Malignant Bilious, or Yellow Fever in Philadelphia (1799). Rush became known for his aggressive and controversial approaches to combatting yellow fever with bleeding and purging. Courtesy Countway Library of Medicine, Harvard University
Lewis and Clark on the Lower Columbia
1803

Lewis and Clark on the Lower Columbia, painting by Charles Marion Russell. Prior to the famous expedition to the West, in 1803 President Thomas Jefferson sent Meriwether Lewis to Philadelphia to meet with Penn medical faculty. Benjamin Rush taught Lewis about frontier illnesses and the procedure for bloodletting; he also provided the Corps of Discovery with a medical kit. Benjamin Smith Barton, professor of natural history, provided expertise on botany and paleontology.
Dissection Kit
1808
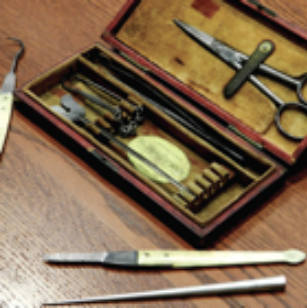
Anatomist Caspar Wistar’s dissection kit, c. 1808. Courtesy Wistar Institute Archives
Notebook of Thomas Chalkley James
1816

Notebook of Thomas Chalkley James, Penn’s first professor of midwifery (separate from anatomy), session of 1816-1817. Of note is the large number of students hailing from Southern states. Courtesy Pennsylvania Hospital Historic Collections, Philadelphia
William E. Horner describes Tensor Tarsi muscle
1824
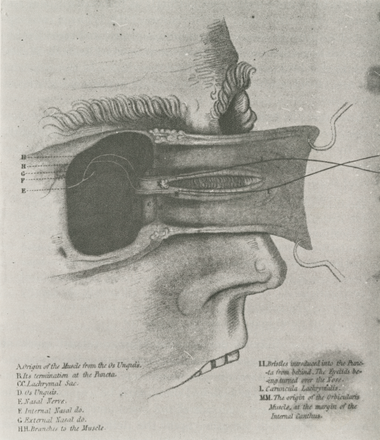
Tensor tarsi muscle (Horner’s muscle), first described by William E. Horner (M 1814) in 1824. Horner was a preeminent anatomist, surgeon, dedicated teacher, and, as dean for an unprecedented three decades, a leader who left his mark on Penn’s medical school.
Architectural scroll
1829

Architectural scroll, an artifact from the faculty room of the 1829 building, carved by Mordecai K. Van Horn.
Ninth Street campus of the University of Pennsylvania
1829

Ninth Street campus of the University of Pennsylvania, Medical Hall (left) and College Hall (right), home of the University, 1829-1872, and its Medical Department, 1829-1873. Medical Hall contained the Anatomical Museum, dissecting laboratories, and three lecture rooms through which students rotated every two hours. Its construction added debt to the medical faculty, stepping up the need for high attendance numbers at their lectures. William Strickland designed the Federal-style buildings. 1830 watercolor by J.G. Caldelaugh
Chemical laboratory and lecture room of Robert Hare
1829

Chemical laboratory and lecture room of Robert Hare, 1831. When the University hired architect William Strickland to design the twin buildings for the Ninth Street campus in 1829, Hare worked with Strickland to create a space that best suited his needs for teaching, research, and demonstrations while providing proper ventilation, heat, and light. Courtesy National Library of Medicine.
Anatomy Museum
1830
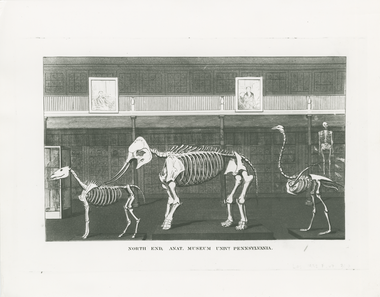
Anatomy Museum. Founded in the first quarter of the 19th century, the museum consisted of Caspar Wistar’s collection, specimens donated by Pennsylvania Hospital, and a substantial addition of specimens provided by William Horner. It was available to medical students two mornings a week and, according to an 1844 catalogue of the Medical Department, was “abundantly furnished with preparations of every kind calculated to give the fullest illustration of a course of Anatomical lectures.”
Roper’s Gymnasium
1831

Roper’s Gymnasium, 274 Market Street, 1831. In 1831, the Trustees entered into an agreement with Roper to admit students one hour each day, under his personal supervision to help avoid accidents, for the discounted annual rate of $10 rather than $20 for gym membership. In return, the Trustees appointed Roper the University’s Teacher of Gymnastics. Courtesy Library Company of Philadelphia.
Philadelphia Hospital
1832

Philadelphia Hospital (later Philadelphia General Hospital), part of the Philadelphia “Blockley” Almshouse, relocated to West Philadelphia in 1832. David J. Kennedy watercolor, 1889. Because students attended lectures all day for two years, it became harder for the faculty to enforce the apprenticeship system for clinical training. Pennsylvania Hospital and Philadelphia Hospital would continue to fill that gap until the University moved to West Philadelphia in the 1870s and opened a hospital of its own. In the interim, medical students rode the omnibuses to Philadelphia Hospital. Courtesy Historical Society of Pennsylvania.
Henry H Smith's Anatomical Atlas
1845
Henry H. Smith’s Anatomical Atlas, Illustrative of the Structure of the Human Body, 1845. The illustration on this title page depicts an anatomical lecture in Medical Hall.
Joseph Leidy
1853

Joseph Leidy (M 1844) brought a different perspective to the professorship of anatomy when he succeeded the late William Horner to the position in 1853. Unlike his surgeon-anatomist predecessors, Leidy took the lectern as a naturalist, one with a formidable reputation at an early age. He had already founded the field of vertebrate palæontology in America and made important discoveries in botany, comparative anatomy, geology, and mineralogy. His work with microscopy advanced the field of public health. Leidy identified the Trichina spiralis in pigs that causes trichinosis and the link between hookworms and pernicious anæmia. In 1853, six years before Charles Darwin published The Origin of Species, Leidy wrote his views on evolution and natural selection; he subsequently recommended Darwin for election to the Academy of Natural Sciences in Philadelphia. Leidy chaired anatomy at Penn’s medical school for nearly four decades while founding and heading the University’s Department of Biology. He served as medical dean from 1877 to 1888. The Laboratory of Biology, built on Hamilton Walk in 1910, bears his name.
Plate from Dermatological Illustration Collection
1871
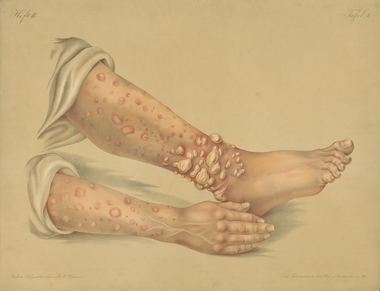
Plate from Dermatological Illustration Collection donated by Louis A. Duhring (M 1867) to the Department of Dermatology in 1913. Duhring, an internationally renowned dermatologist who helped establish dermatology as a specialty in the United States, would have used this collection of 588 folio-size lithographs and 844 photographs as a teaching tool.
Penn Medical Hall
1874

Medical Hall, primary home for Penn’s medical school from 1874 to 1904.
Penn’s West Philadelphia campus
1874

The original three buildings of Penn’s West Philadelphia campus (from left to right): University Hospital, College Hall, and Medical Hall (on the far side of College Hall). The buildings to the right fronted Woodland Avenue, today’s Locust Walk.
Medical Class on the steps
1879

Medical Class of 1879 on the steps of Medical Hall.
Nathan Francis Mossell
1882

Nathan Francis Mossell (M 1882), the first black graduate of Penn’s medical school. Mossell was instrumental in founding the Frederick Douglass Memorial Hospital and Training School, where he served as medical director for 47 years.
Medical faculty, fall
1885

Medical faculty, fall 1885 - spring 1889. Provost William Pepper Jr., holding the revered professorship of theory and practice of medicine, appears in the center. Clockwise from the top right: Richard A.F. Penrose (M 1849), professor of obstetrics and diseases of women and children; William Goodell (M 1871), professor of clinical gynecology; Horatio C. Wood Jr. (M 1862), professor of materia medica, pharmacy and general therapeutics; John Ashhurst Jr. (M 1860), professor of clinical surgery; Edward Tyson Reichert (M 1879), professor of physiology; William Osler, professor of clinical medicine; Theodore George Wormley, professor of toxicology and chemistry; James M. Tyson (M 1863), professor of general pathology and morbid anatomy; David Hayes Agnew (M 1838), the John Rhea Barton Professor of Surgery and Clinical Surgery; Joseph Leidy (M 1844), professor of anatomy.
Property Atlas of Philadelphia
1886
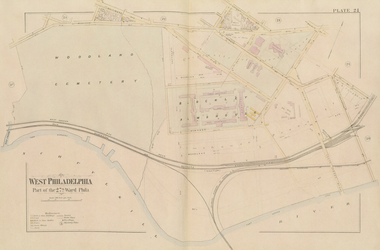
Property Atlas of Philadelphia, 1886, plate 24, showing the early West Philadelphia campus buildings and the neighboring Blockley Almshouse south of Pine Street. The Almshouse complex included Philadelphia Hospital (later Philadelphia General Hospital), where Penn medical faculty cared for the city’s poor and Penn medical students supplemented their clinical training.
William Osler conducting a demonstration at the Blockley Mortuary
1887

William Osler conducting a demonstration at the Blockley Mortuary, c. 1887. Courtesy Osler Library of McGill University
The Agnew Clinic
1889
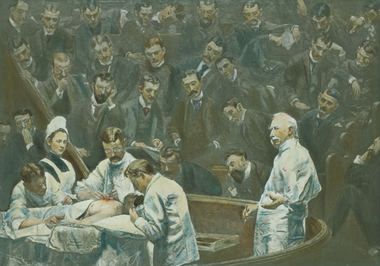
The Agnew Clinic, painting by Thomas Eakins commissioned by the Medical Class of 1889, whose portraits appear as the onlookers. Eakins depicted D. Hayes Agnes wearing a gown in the new age of antisepsis
Pathology laboratory in Medical Hall
1890

Pathology laboratory in Medical Hall, c. 1890.
Charles Lester and Mary McNally
1896

Charles Lester Leonard and nurse Mary McNally, Roentgenologic (Radiology) Department in the Surgical Dispensary, 1896. Leonard pioneered the specialty of radiology in the United States. Collections of the late Nadine Landis, Courtesy Trustees of the University of Pennsylvania
Sensory root of the Trigeminus
1901
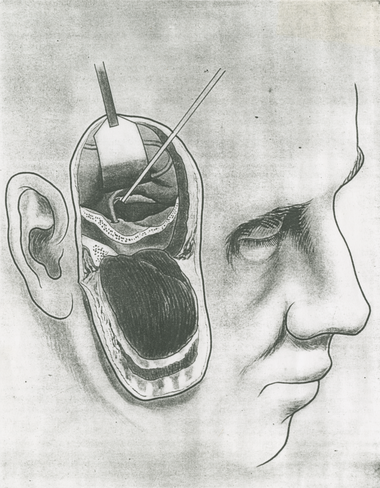
Division of the sensory root of the trigeminus for the relief of trigeminal neuralgia or tic douloureux. Charles H. Frazier developed this procedure for pain relief with neurologist William Spiller in 1901. During the course of his surgical career, Frazier performed this operation more than 700 times.
Medical Laboratories Building Erected
1904

Medical Laboratories Building, erected on Hamilton Walk, 1904. Physiology, pharmacology, and pathology moved from the Victorian-style Medical Hall into this modern building. Anatomy and chemistry would remain in the Hare Building until the Anatomy-Chemistry wing was added in 1928.
Mask and Wig Club
1905

Medical students performing in the Mask and Wig Club. As an undergraduate, Charles H. Frazier (M 1892) was a founder of this all-male revue. Renowned poet and author William “Billy” Carlos Williams (M 1906), shown here as “Polonius” in the 1905 production of “Mr. Hamlet of Denmark,” also was a member of the varsity fencing team.
Medical Ward Class
1906

Medical ward class, c. 1906. Ward classes consisted of bedside training in which an instructor demonstrated cases to small groups of five to ten students. Fourth-year students also assisted resident physicians in the wards of the University Hospital.
Dean William Pepper III
1912

Dean William Pepper III (M 1897), c. 1920. As dean from 1912 to 1945 and a father figure to many students, Pepper steered the school through lean times and helped students through the difficult strains of the Depression.
Barton Cooke Hirst Amphitheater
1920
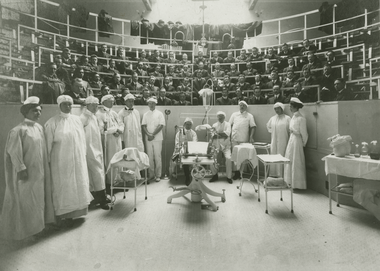
The clinical amphitheater of Barton Cooke Hirst (M 1883), c. 1920. Hirst, who headed the Department of Obstetrics for 38 years (1889-1927), ushered the University Hospital into the modern age of obstetrics. He founded a maternity hospital and, in so doing, advanced obstetrical education for medical students from textbook and manikin demonstrations to hands-on experience with deliveries.
Elizabeth Kirk Rose
1926

Elizabeth Kirk Rose (M 1926, GME 1930). Even in the 1960s, Rose preferred to use her bicycle to commute from the train station to campus. When she did her internship at HUP, Rose was the only woman out of 28 house staff. For two decades she served on the Penn pediatrics faculty, as well as on the staff of CHOP and Presbyterian Hospital. From 1950 to 1956, Rose headed the Division of Maternal and Child Health in the Philadelphia Department of Public Health. In 1956, she joined Penn’s Department of Community Health and helped lay the groundwork for involving medical students and residents in community-based learning and outreach. An advocate for women, in 1962 Rose organized a picnic for female medical students and alumnae that evolved into the annual Elizabeth Kirk Rose Women in Medicine Dinner. She received the Distinguished Graduate Award and the Lindback Award for Distinguished Teaching
Alfred Newton Richards
1929

Alfred Newton Richards and pupils at the International Physiological Congress, 1929. These are just some of Richards’s protégés who trained in his laboratory and then attained fame in their own right. Seated: A.N. Richards. Standing (left to right): Arthur Walker, Leonard Bayliss, Isaac Starr, Joseph T. Wearn, Carl F. Schmidt. Cecil K. Drinker, Oscar Plant, John Barnwell, A.E. Livingston, Joseph Hayman, and Howard Florey.
Penn Campus Aerial View
1934

Aerial view of the Penn campus, 1934, looking southwest toward HUP and the enormous Philadelphia General Hospital complex, future site for the expansion of the medical school’s facilities and the Children’s Hospital of Philadelphia.
Christian J. Lambertsen
1941

While a Penn medical student, Christian J. Lambertsen (M 1943), an expert on respiratory physiology, invented the Lambertsen Amphibious Respirator Unit, or LARU, forerunner of today’s scuba technology. During World War II, Lambertsen joined the Army Medical Corps and was recruited by the Office of Strategic Services to train its maritime unit to use his underwater breathing device.
Marriage Council of Philadelphia
1948

Young couple meeting with Emily Hartshorne Mudd at the Marriage Council of Philadelphia (soon to become part of Penn Psychiatry’s Division of Family Study), 1948. A champion of women’s rights and a pioneer in marriage counseling and family studies, Mudd became the School of Medicine’s first woman to be named a full professor in 1956. Her appointment was in the Department of Psychiatry; she also worked with the Department of Obstetrics and Gynecology. Mudd joined William Masters and Virginia Johnson as a consultant on counseling techniques and, in her 70s, commuted to St. Louis to assist them with their study on the prevention of sexual dysfunction. Courtesy Special Collections Research Center, Temple University Libraries, Philadelphia, PA
Conference with Surgical Faculty
1950

I.S. Ravdin in conference with surgical faculty, early 1950s. (Left to right) Front row: unknown, Jonathan Rhoads, Boland Hughes, Julian Johnson. Back row: William Fitts, Cletus Schwegman, Harold Zintel, Henry Royster.
Gold Medalists Olympic Games
1952

Gold medal winners in sailing at the 1952 Olympic Games in Helsinki. Britton Chance (third from left), director of the Eldridge Reeves Johnson Foundation for Medical Physics, designed and steered the boat. Chance’s interest in sailing and science went back to his childhood; at age 15 he invented an automatic steering device for ships.
Karyotype
1960
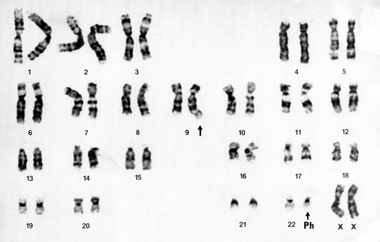
Karyotype for the Philadelphia chromosome, showing the small and defective chromosome. Peter C. Nowell (M 1952) and David Hungerford’s discovery, made in 1960, first linked cancer to a genetic abnormality.
Alfred Newton Richards Building
1962

Alfred Newton Richards Building, view from the bio pond, c. 1965. Designed by architect Louis I. Kahn, the modern research tower was completed in 1962. As research was becoming more collaborative, Kahn’s design broke from the tradition of the impersonal double-loaded corridor plan to the more humanistic cluster of small labs, forming a “scientific village” that linked the biological and medical sciences and allowed investigators to interact in communities.
A Meeting of the Minds
1962

A conversation between Aaron T. Beck and the Dalai Lama, “A Meeting of the Minds,” International Congress of Cognitive Psychotherapy, Göteborg, Sweden, 2005. Beck, “the father of cognitive therapy,” introduced cognitive behavioral therapy in 1962.
Department of Medicine Chair
1965
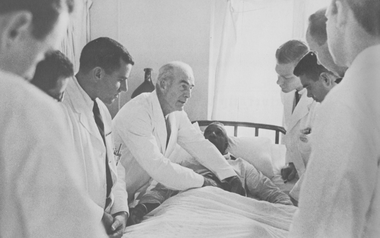
Francis C. Wood, chair of the Department of Medicine (1947-1965), conducting ward rounds, 1965.
Medical Students
1965

Medical students taking a break from the grind, 1965.
Mildred Cohn
1970

Mildred Cohn, the first scientist to distinguish the three phosphorous atoms of ATP, discussing the spectra run on Penn’s 220 megahertz nuclear magnetic resonance spectrometer with investigators from Johns Hopkins University School of Medicine and the Institute for Cancer Research, 1970. This was the most powerful model of its time and the first in a medical school on the East Coast. Penn acquired the spectrometer to be shared with regional institutions, with Cohn as the principal investigator and John S. Leigh Jr. directing the magnetic resonance facility. Photo: Frank Ross
Surgeon Leonard Miller
1972
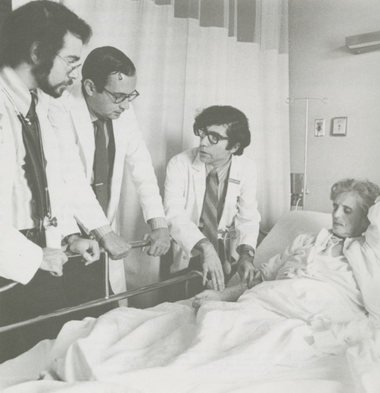
Surgeon Leonard Miller (center) discusses post-operative symptoms with first-year students in a new program providing close contact with patients and physicians from their first day in medical school, 1972. Following a two-year pilot program, as of fall 1971 all first-year students had exposure to clinical medicine in conjunction with basic science courses.
Koop Separates Conjoined Twins
1974

C. Everett Koop with Clara and Altagracia Rodriguez, conjoined twins from the Dominican Republic, joined together at the lower trunk and pelvis with partially united gastrointestinal urinary and reproductive systems. In 1974, Koop and a team of 26 doctors and nurses at CHOP separated the twins. Courtesy The Children’s Hospital of Philadelphia
Penn Medical Students
1974

Medical students and families, 1974. In 1973, 12 percent of Penn medical students were women and seven percent were minorities. Because of cuts in federal funding and increased reliance on state subsidies, the percent of Pennsylvanians in each entering class was targeted to increase from 40 to 50 percent.
John Glick
1977
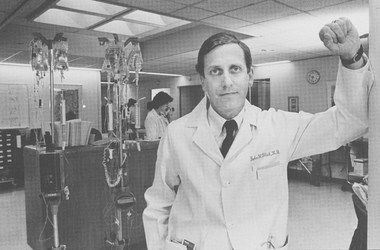
John Glick, professor of medicine, director of the University of Pennsylvania Cancer Center, and a national expert on breast cancer and Hodgkin’s disease, 1986. Penn’s Cancer Center and Department of Radiation Therapy (now Radiation Oncology) began making lumpectomy and radiation therapy available in 1977 as an alternative to mastectomy, with the equivalent results in curing early-stage breast cancer. The broader medical community would accept this approach in 1985.
James A. Hoxie
1982

James A. Hoxie, cover of The Pennsylvania Gazette, May 1988. When AIDS patients started coming to HUP in 1982, Hoxie’s lab took on the task of testing for the T cell deficiency. He shifted his research from cancer to T4 lymphocytes, the structure of the viral envelope, and how daughter viruses mutate in T cells with the hope of gaining enough of an understanding of the structure and life cycle of the virus to begin developing a vaccine. Photo: Eugene Mopsik
Starting Here, Starting Now
1983

“Starting Here, Starting Now,” Spoof ’ 1983.
Jillian Elizabeth Johnston
1983

Jillian Elizabeth Johnston, born September 23, 1983, the first child conceived and born through HUP’s in vitro fertilization (IVF) program. Luigi Mastroianni Jr.’s groundbreaking research in the mid-to-late 1970s paved the way for IVF.
Clinical Research Building
1989

Clinical Research Building (CRB), Curie Boulevard, completed 1989. This new building marked the start of the University’s medical campus expansion onto the former PGH site. Other than the auditorium, CRB was the medical school’s first building exclusively dedicated to research space since the Richards Building (now Richards Medical Research Laboratories) of nearly three decades earlier.
William N. Kelley
1989

William N. Kelley, executive vice president of the University, dean of the School of Medicine, and chief executive officer of the Medical Center and later the Health System. Kelley came to Penn as a world leader in the study of purine metabolism, a pioneer in the field of clinical genetics, and a proven builder of programs, facilities, and faculty from his tenure as the University of Michigan’s chair of Internal Medicine. At Penn, he created the prototype of an academic, integrated delivery system, a network of physician practices, hospitals, and other clinical settings that provided continuous training settings for medical students and residents. Kelley brought Presbyterian Hospital, and Pennsylvania Hospital, and multispecialty facilities under the University of Pennsylvania Health System umbrella. Research programs exploded at Penn with Kelley’s ability to attract talented investigators and funding and to build laboratory facilities. He led the medical school to new heights in research income and overall rankings and oversaw the development of a new curriculum for the 21st century.
21st Century Endowed Scholars Program
1996

In 1992, Walter Gamble (M 1957) and his wife, Anne, established the 21st Century Endowed Scholars Program so that Penn Medicine students could have the freedom to pursue the medical careers of their choice without being constrained by financial concerns. It was only in 1996 that the identities of these visionary donors were revealed. Since its beginnings, as the debt borne by medical students has continued to rise, the program has covered the full four-year tuition of more than 220 students. The Gambles are shown surrounded by many of the medical students they have supported over the years.
Abramson Cancer Center
1997

Madlyn and Leonard Abramson. In 1997, the Abramsons gave a $100-million gift that kick-started Penn’s present-day cancer research powerhouse, known as the Abramson Cancer Center. In 2010, they gave an additional $25 million to support continued basic science and translational research progress in the Abramson Family Cancer Research Institute, which is among the nation’s preeminent incubators for discovery of new diagnostic tools and novel therapies.
Lancelot
2001

Lancelot, the first dog to enjoy stable reversal of blindness after a single subretinal injection of AAV.RPE65. In 2001, Jean Bennett, Albert Maguire,and a team of researchers from Penn, Cornell University, and the University of Florida used gene therapy to restore sight in dogs afflicted with a variation ofLeber congenital amaurosis (LCA). Seven years later, Bennett and Maguire conducted a clinical trial at CHOP on three young adults with CLA and safely restored their vision using gene therapy.
Brain Behavior Laboratory
2002
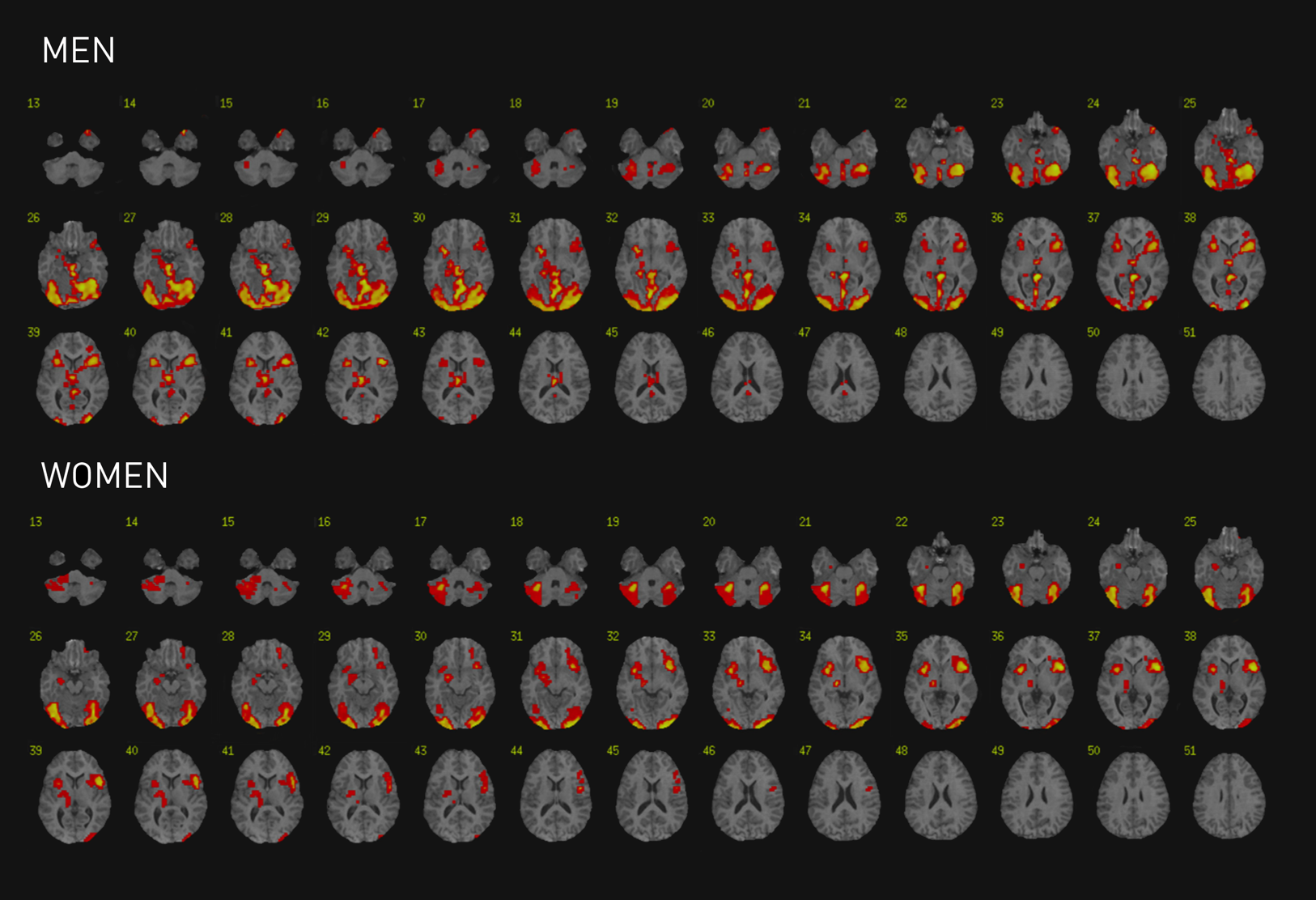
These fMRI scans, drawn from the research of psychologist Ruben C. Gur, director of Penn’s Brain Behavior Laboratory, and psychiatrist Raquel E. Gur (M 1980; GME 1984), show more activity among men’s brains as they try to identify emotions, needing to activate large neural networks; in contrast, women activate a more circumscribed amygdala-cortical system.
Robot Wrist
2004

Robot wrist. The robot instrument closely mimics the human wrist while providing increased freedom in motion and rotation. In 2004, Bert W. O’Malley Jr. and Gregory S. Weinstein co-founded the world’s first human robotics head, neck, and skull base surgery program, developing novel surgical procedures collectively called TransOral Robotic Surgery (TORS). In 2009, the FDA approved the use of the da Vinci surgical system to perform TORS for selected malignant lesions of the throat and voice box as well as all benign disease. Courtesy da Vinci
Fibrodysplasia Ossificans Progressiva
2006
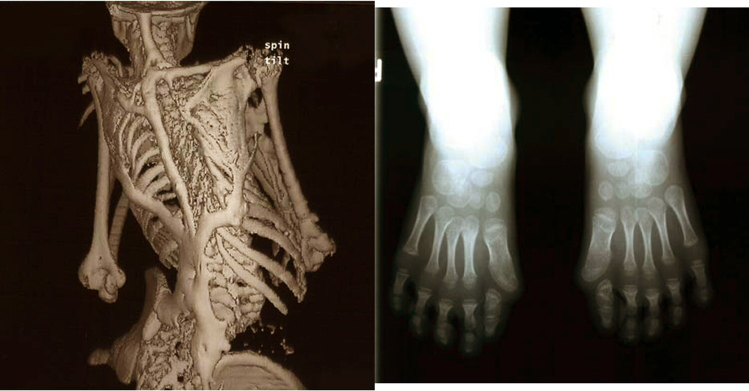
Characteristic clinical features of fibrodysplasia ossificans progressiva (FOP), a rare disease that causes soft tissue to turn to bone, eventually immobilizing patients. In 2006, Frederick Kaplan, Eileen Shore, and colleagues discovered the genetic mutation that causes FOP. This discovery is important not only for FOP patients, but may also lead to new therapies for more common skeletal conditions.
Simulation Training
2007
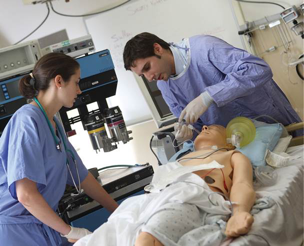
Simulation training became part of medical students’ educational experience in 2007. As fewer patients have been admitted for inpatient care, procedural experience on real patients has become more limited for students. Simulation training has helped fill that gap.
J. Larry Jameson
2011

J. Larry Jameson, executive vice president of the University of Pennsylvania for the Health System and dean of the School of Medicine, 2011- . Photo: Sabina Louise Pierce
Perelman Center for Advanced Medicine
2011

The Ruth and Raymond Perelman Center for Advanced Medicine (PCAM) and Smilow Center for Translational Research, Civic Center Boulevard, built 2006-2011. These physically integrated buildings house the Abramson Cancer Center, Penn’s Department of Radiation Oncology and the Roberts Proton Therapy Center, cardiovascular medicine, and an array of other specialties, as well as an outpatient surgical pavilion. The 531,000-square-foot Smilow Center houses state of-the-art research space to support bench-to-bedside medicine.
Penn's School of Medicine is renamed
2011

Raymond and Ruth Perelman, who contributed $225 million to Penn’s School of Medicine. In recognition of this transformative gift, the medical school was renamed as the Raymond and Ruth Perelman School of Medicine at the University of Pennsylvania in 2011.
Modified T Cell Therapy
2011
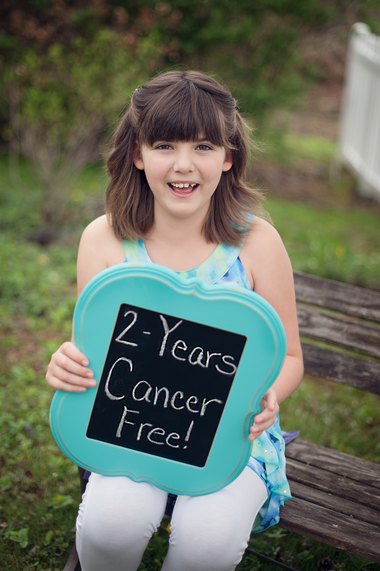
In 2011, Carl June and colleagues used a disabled form of HIV as a vector to reprogram this young girl’s immune system to kill her leukemia cells. Pictured here two years later, she was the first pediatric patient to receive this modified T cell therapy. Photo: Kari Whitehead
Lewy Body
2014
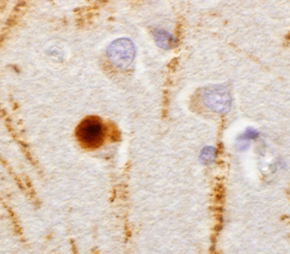
Lewy body (brown) in human tissue with Parkinson’s disease (PD), 2014.Virginia M.-Y. Lee (MBA 1984), John Q. Trojanowski (GME 1980) and colleagues identified α - synuclein as a protein in Lewy bodies, the hallmark of PD, and TDP-43, a protein involved in amyotrophic lateral sclerosis. More recently, they found that misfolded α - synuclein can be transmitted from cell to cell in mouse models and are applying this discovery toward finding a treatment for people with PD.
Daniel Rader's Research
2014
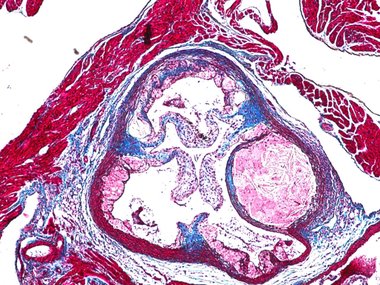
From Daniel Rader’s research, mouse aorta showing cholesterol deposition (pink crystal-like mass in sphere) to the right of an atherosclerosic lesion, smooth muscle cells (red) and cardiac muscles. Collagen tissue is blue. An international leader in the human genetics of lipoprotein biology and cardiovascular disease, Rader has a strong translational interest in developing novel therapies to regulate cholesterol.
Henry A. Jordan M’62 Medical Education Center
2015

Workers on the beam building the Henry A. Jordan M’62 Medical Education Center at the eastern edge of the Penn campus, 2014. The Jordan Center opened in 2015. The high-technology center, designed to facilitate the type of learning envisioned in Curriculum 2000®, is physically integrated with both the Smilow Center for Translational Research and the Perelman Center for Advanced Medicine, making it one of the first in the nation to place education facilities in the midst of active clinical care and research lab space. For the first time, students at work in the classroom find themselves connected to the dynamic practice of both medicine and biomedical research. Photo: Daniel Burke
