Penn Sleep Medicine Clinical Fellowship
Welcome to the Penn Sleep Medicine Clinical Fellowship!
The Sleep Division in the Department of Medicine at the University of Pennsylvania was the first independent multi-disciplinary sleep medicine program. This medical school-wide program has trained many leaders in sleep medicine and sleep research across the country for decades. The program has been deemed by the National Academy to be the prototype for a successful program.
As an independent Division of Sleep Medicine within the Department of Medicine comprised of renowned, multidisciplinary expert faculty, Penn is uniquely positioned to provide exceptional training in academic sleep medicine.
The fellowship also offers additional specialty training in Pediatric Sleep Medicine at the Children's Hospital of Philadelphia (CHOP) under Nancy Lin, MD, in Sleep Surgery under Raj Dedhia, MD, at the Philadelphia Veteran's Administration Medical Center (VAMC) under Samuel Kuna, MD, as well as numerous other clinical and research opportunities with our Sleep Medicine faculty.
From all of us, thank you for your interest in the University of Pennsylvania Perelman School of Medicine (PSOM) Sleep Medicine clinical fellowship!



Indira Gurubhagavatula, MD Maria Antoniou, MD Jennifer Dorsch, MD
Professor of Medicine Associate Professor of Clinical Medicine Assistant Professor of Clinical Medicine
Director, Sleep Medicine Fellowship Associate Director, Sleep Fellowship Associate Director, Sleep Fellowship
Our 12-month ACGME-accredited clinical fellowship program offers an outstanding comprehensive curriculum designed to prepare physicians to become exceptional board-certified specialists in academic sleep medicine. Trainees complete rotations in numerous settings including the University of Pennsylvania Health System, Philadelphia VA Medical Center, and the Children’s Hospital of Philadelphia.

The program also emphasizes research opportunities to further equip physicians interested in becoming independent investigators. After the initial year, fellows may go on to pursue a 2-3 year postdoctoral research fellowship in one of four distinct tracks (Basic Science, Patient-Oriented Research, Clinical Epidemiology, Translational Research, Health Policy, & Medical Education).
Penn Sleep Medicine Fellowship Program offers 4 tracks in Sleep Medicine: Adult Sleep Medicine, Psychiatry, Otorhinolaryngology, and Pediatric Sleep Medicine.
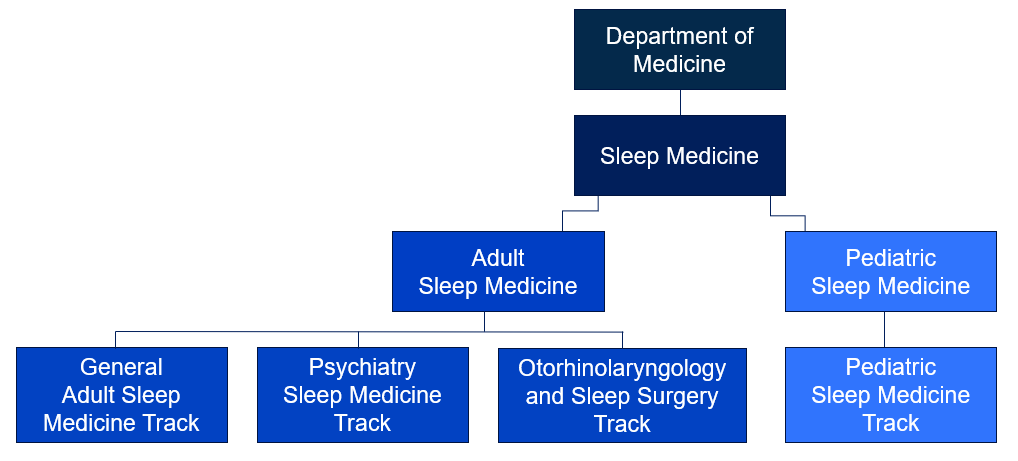
The Pediatric Sleep Medicine track is run in conjunction with the Children's Hospital of Philadelphia (CHOP) under CHOP site director Nancy Lin, MD. The Otorhinolaryngology and Sleep Surgery track site director is Raj Dedhia, MD. and Psychiatry track site director is Subhajit Chakravorty, MD.
Our graduates have achieved a 100% board pass rate and are consistently successful in securing desired positions across the country. Furthermore, countless alumni go on to become leaders in the field of sleep medicine.
Applicants to the sleep fellowship-training program are required to have completed a residency in internal medicine, neurology, otolaryngology, pediatrics, psychiatry, family medicine or anesthesiology. Individuals with subspecialty training such as pulmonary medicine are encouraged to apply.
The University of Pennsylvania Sleep Medicine Fellowship Program participates in the National Residency Matching Program (NRMP). Applications will ONLY be accepted through the Electronic Residency Application Service (ERAS).
General documents required for application include:
- Curriculum Vitae
- Personal Statement
- Three Letters of Recommendation (one must be from the applicant's most recent Program Director)
- USMLE Transcript
- Medical Student Performance Evaluation (MSPE) or Dean's Letter
- Medical School Transcript
- ECFMG Status Report, if applicable
The Sleep Medicine Fellowship Program adheres to the deadlines of the ERAS and NRMP fellowship match cycle. A sample timeline is below, and we encourage you to check the ERAS and NRMP websites for additional information including specific instructions and timelines for applications and match dates, respectively.
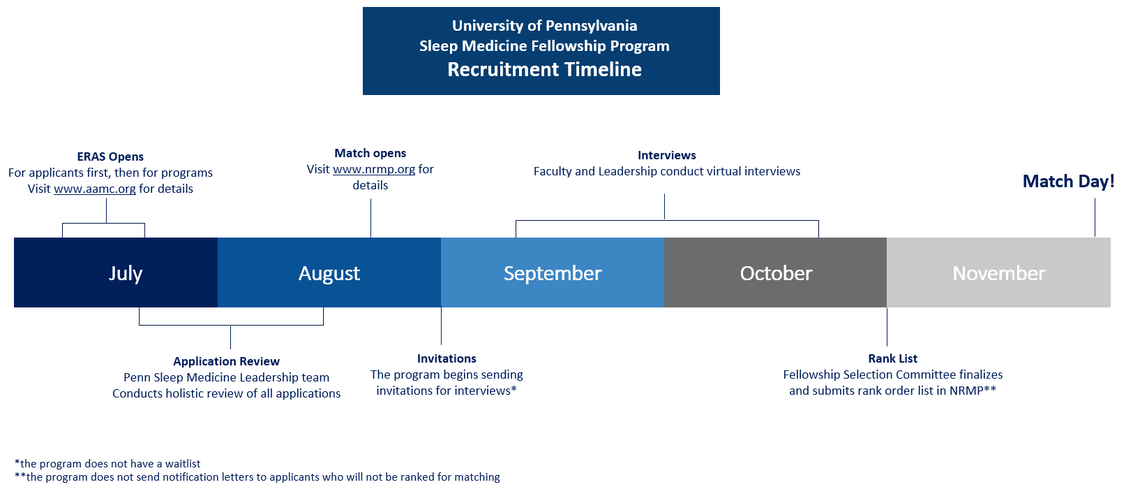
Given the multidisciplinary structure of the program, the fellowship curriculum is tailored to allow each trainee to concentrate on a particular area of specialization, i.e. pediatric or adult sleep medicine, through established tracks.
Under ACGME guidelines, each fellow is required to complete a core curriculum that meets the minimum requirements for clinical training in both adult and pediatric sleep medicine while allowing flexibility to concentrate further in a particular area of interest.
Both pediatric and adult track fellows participate in the initial intensive Summer Lecture Series followed by weekly Fellows Educational Series throughout the year.
For pediatric track trainees, this will require:
- Outpatient pediatric sleep medicine experiences at CHOP
- Outpatient and inpatient adult sleep medicine experiences spread over the University of Pennslyvania Health System (UPHS) and Philadelphia VAMC sites
- Continuity practice experiences in both adult and pediatric sleep medicine
- Review of polysomnography and other sleep-related diagnostic studies
- Additional electives to allow for a concentrated experience in sleep disorders in children
For adult track trainees, this will require:
- Outpatient and inpatient adult sleep medicine experiences spread over the UPHS and Philadelphia VAMC sites
- Outpatient pediatric sleep medicine experiences at CHOP
- Continuity practice experience in adult sleep medicine*
- Review of polysomnography and other sleep-related diagnostic studies
- Elective time to allow for a concentrated experience in sleep disorders in adult
Sample Schedules and Example Track Options
Note that all fellows participate together in the Summer Lecture Series during the first month of the fellowship.
Added Educational Opportunities and Track Options:
*Adult track trainees can also request an optional second continuity practice experience in Pediatric Sleep Medicine.
*Trainees also may request additional Otolaryngology and Sleep Surgery experiences.
*Trainees may request additional Insomnia (CBT-I) and Behavioral Sleep Medicine experiences.
*Trainees may request additional experiences in Hypoventilation and NIV management.
a60
Basic and enhanced educational training in the diagnosis and management of Hypoventilation Syndromes and NIV Management is highlighted in Penn’s Sleep Medicine fellowship training. The basis of the added Hypoventilation/NIV track is intensive education regarding pulmonary physiology and the effects of noninvasive positive pressure ventilation on different disease states. The fellow will receive training in initiation and titration of noninvasive positive pressure ventilation for efficacy and patient comfort. To accomplish this, an in-depth understanding of BPAP and ventilator algorithms will be taught, and the fellow will be able to utilize adjunctive measures of CO2 monitoring to ensure ventilatory optimization. Education regarding sleep study evaluation for hypercarbia using end tidal carbon dioxide and transcutaneous carbon dioxide measurements will be emphasized. Training locations include outpatient clinics and a robust inpatient hospital consult service experience.
Research Opportunities for Sleep Fellows
We are fortunate that Penn has one of the most vibrant and comprehensive sleep and circadian research programs in the world, with numerous leaders in basic sleep and circadian research and some of the most impactful translational researchers. We have the opportunity to train fellows who are interested in research but have less of a background in research. Through our various training grants, opportunities to obtain masters' degrees, and our dedicated multi-disciplinary faculty, we are committed to helping our post-doctoral fellows achieve academic success.
5704Clinical faculty interests and recent publications may be found on their individual Sleep Faculty pages, or using examples found in a "Recent Selected Penn Sleep Publications" link. Penn Sleep and CSI Research Labs are listed below.
Featured Sleep Fellow Alumni Researcher: Toshihiro Imamura MD, 2019-2020 Sleep Fellow
 Dr. Imamura is a clinician and researcher at the Children’s Hospital of Philadelphia. The title of Dr. Imamura’s research is “Anesthesia and Sleep: Mechanisms of Generating Two Similar Yet Distinct Unconscious States in the Brainstem” (R35 through NIGMS (MIRA-ESI: https://grants.nih.gov/grants/guide/pa-files/PAR-23-145.html). Description: The network in the brain that controls sleep and wakefulness is turned on during general anesthesia, but it is unknown how the brain can produce coma and sleep, two unconscious states that are similar but different, by turning on the similar brain network. This project will look at both the same and different parts of the brain network that are active during anesthesia and sleep by using state-of-art techniques that give exact information about each cell and compare two brain networks side by side. The proposed project is important for public health because it will lead to better clinical care for people who need unconsciousness as a treatment, including general anesthesia, sedation during procedures, and insomnia.
Dr. Imamura is a clinician and researcher at the Children’s Hospital of Philadelphia. The title of Dr. Imamura’s research is “Anesthesia and Sleep: Mechanisms of Generating Two Similar Yet Distinct Unconscious States in the Brainstem” (R35 through NIGMS (MIRA-ESI: https://grants.nih.gov/grants/guide/pa-files/PAR-23-145.html). Description: The network in the brain that controls sleep and wakefulness is turned on during general anesthesia, but it is unknown how the brain can produce coma and sleep, two unconscious states that are similar but different, by turning on the similar brain network. This project will look at both the same and different parts of the brain network that are active during anesthesia and sleep by using state-of-art techniques that give exact information about each cell and compare two brain networks side by side. The proposed project is important for public health because it will lead to better clinical care for people who need unconsciousness as a treatment, including general anesthesia, sedation during procedures, and insomnia.
Penn Sleep and CSI Research Labs:
Examples of the diverse circadian, genetic, metabolic, and clinical research lab opportunities are listed below.
Pediatric (CHOP), School of Nursing, and other University of Pennsylvania school opportunities also are available (not listed).
--Pack Lab (Medicine): Identifying genes underlying sleep disorders and sleep.
--Naidoo Lab: Understanding how aging affects sleep and the role of sleep in proteostasis.
--Veasey Lab (Medicine): Defining lasting injury to the brain from sleep disorders and identifying the underlying mechanisms.
--Schwab Lab (Medicine): Understanding the contributions of pharyngeal dynamics to sleep disordered breathing.
--Anafi lab (Medicine): Computational approaches to circadian rhythms, neurodegeneration and sleep.
--Rosen Lab (Medicine): Strategies to increase access to sleep medicine therapies in primary care.
--Lazar lab (Medicine): Circadian rhythms and metabolism.
--Fitzgerald lab (Medicine): Circadian rhythms and metabolism.
--Raizen lab (Neurology): Understanding sleep and fatigue.
--Sehgal lab (Neuroscience): Mechanisms of sleep and circadian rhythms.
--Chung lab (Neuroscience): Molecular and neural mechanisms of sleep.
--Weber (Neuroscience): Circuit mechanisms of sleep; special emphasis on REM sleep mechanisms and function.
--Kelz/Proekt lab (Anesthesiology): Mechanisms of unconsciousness.
-- Reddy lab (SPATT): Ancient mechanisms of circadian rhythms.
--Weljie lab (SPATT): Metabolic approaches to understanding sleep.
--Skarke lab (SPATT): Multi omic circadian rhythms in the real world.
--Kayser lab (Psychiatry): Mechanisms and function of sleep during ontogeny and in aging.
--Basner lab (Psychiatry): Effects of the bedroom environment and sleep. Space travel and sleep.
--Gehrman lab (Psychiatry): Biological basis of insomnia.
--Perlis lab (Psychiatry): Insomnia and fatigue.
--Dehdia lab (ENT): Surgical approaches for treating sleep apnea.
--Grant lab (Pediatrics): Genomic mechanisms of sleep disorders.
--Cielo lab (Pediatrics): Evaluation and mechanisms of sleep apnea in children.
--Xanthopoulos: Development, implementation, and adherence to medical and lifestyle interventions, including non-invasive ventilation (CPAP/BPAP), eating habits, physical activity, and sleep.
Full list of all previous Penn Sleep Medicine Fellow Alumni
Graduation 2025

Back row: Nataly Sanchez-Solano MD, Brandon Jones MD, Hannah Wang MD, Vasiliki Triantafillou MD ; Front row: Manju Pillai MD, Ravali Inja MD, Phoebe Yu MD
The Penn Sleep Medicine Fellowship Program prioritizes fellows’ success and wellness. We offer a dynamic curriculum which can be adjusted to reflect your unique interests. Schedules are robust, yet flexible and we build in scholarly and academic time so fellows have time to focus on their interesting academic and research projects. Our distinguished faculty and dedicated program leadership team provide mentorship and a supportive learning environment in which fellows can grow and thrive.
For more information about the University of Pennsylvania & Philadelphia please visit the links below:

Please feel free to contact us with any inquires or questions about our program or the application process.
Penn Sleep Fellowship Coordinator
215-615-0980
PennSleepMedicineFellowship@pennmedicine.upenn.edu
And follow us on Twitter





